What Are Herniated Discs?
Our body is chiefly supported with a spinal column, that is why we can stand upright, bend and twist our body with no injury to our spinal cord. A healthy spine is supposed to have strong muscles and bones, flexible tendons and ligaments, as well as sensitive nerves. However, in case any element in the spine is affected with strain, injury, or disease, this is likely to be the reason for pains.An intervertebral disc separates and serves as a cushion for each vertebra in the spine, therefore the bones are not worn out. Discs can be compared with a radial car tire in their design. Like a tire tread, the outer ring, which is called the annulus, has crisscrossing fibrous bands. These bands are located between vertebrae. The nucleus, which is in the center filled with gel, like a tire tube, is inside the disc.
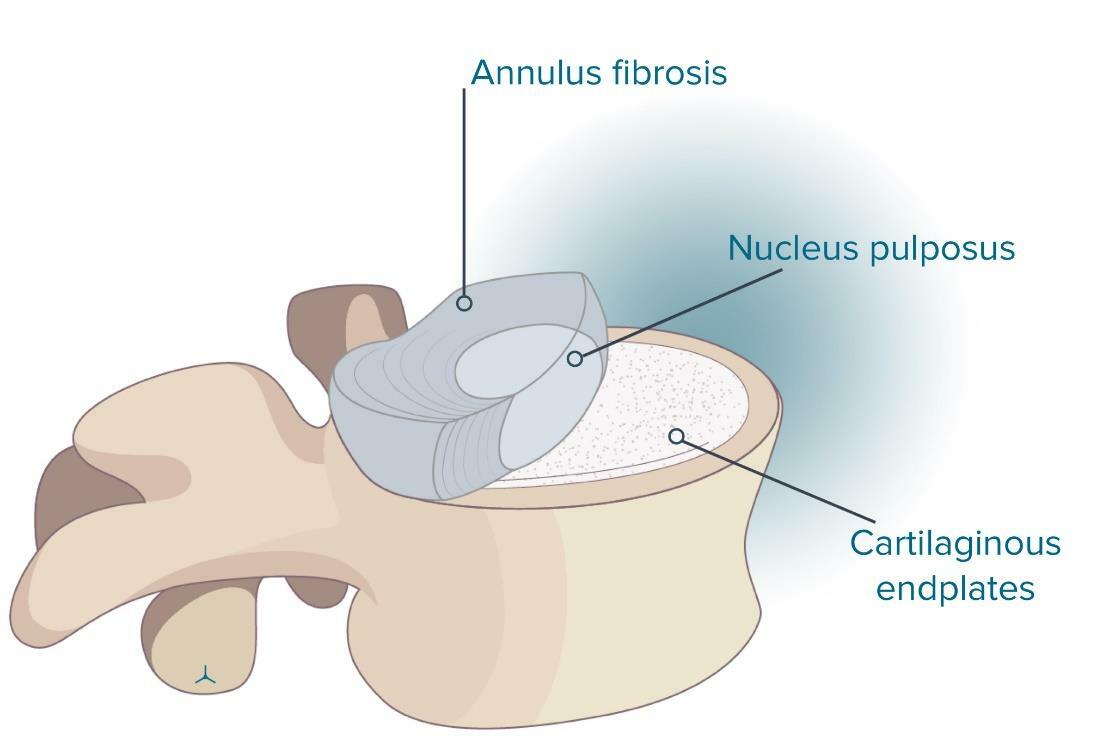
As a part of the aging process, spinal discs could not extensively reabsorb fluid, thus they tend to become brittle and flatter. Injury and strain can bulge or degenerate discs, in other words, the discs achieve the condition when the nucleus pushed out through the annulus affects the nerve roots, which brings a pain in the back.
Difference between bulging and herniated disc
Disc problems could be described in different terms. For example, a herniated disc (sometimes this term can be misspelt like herneated disk ), sequestration, bulging disc, protrusion, raptured disc, slipped disc, thinning disc, degenerative disc, sciatica, etc. Below we describe the main terms and the difference between them.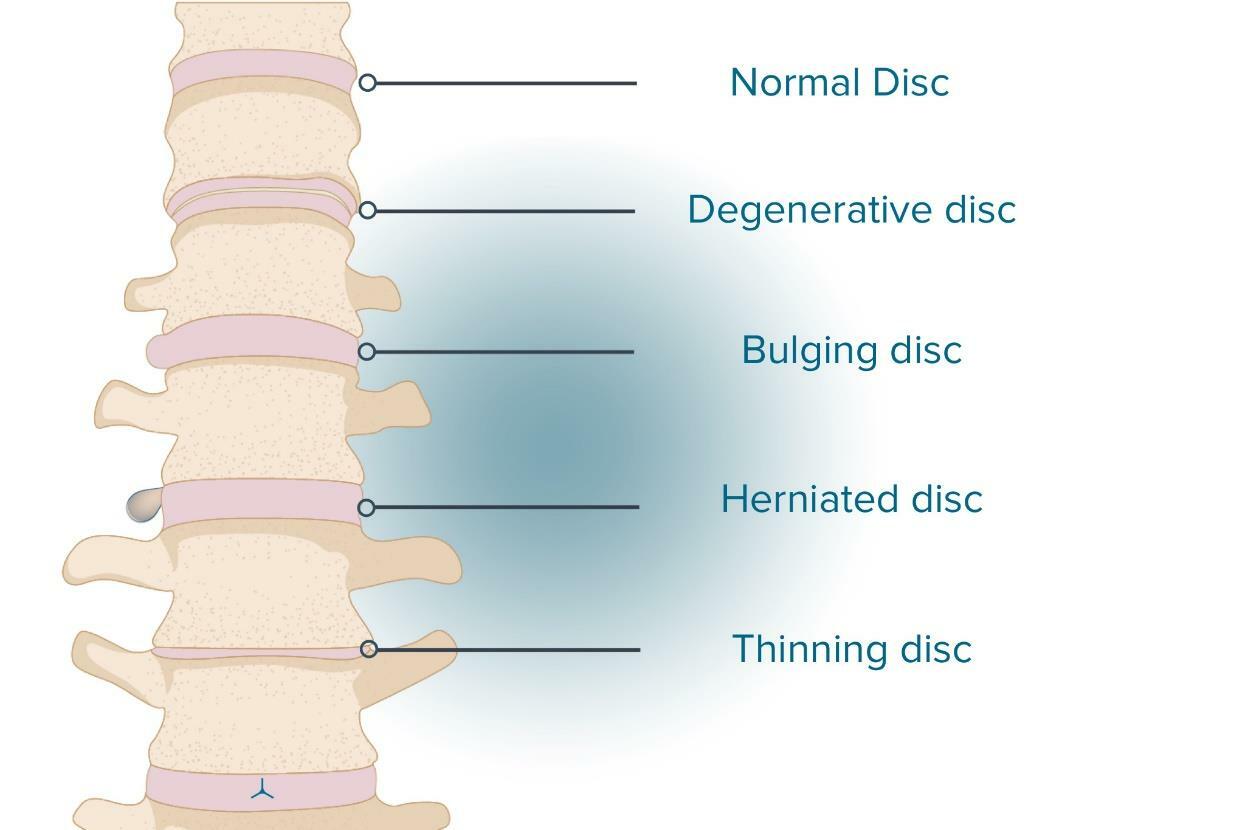
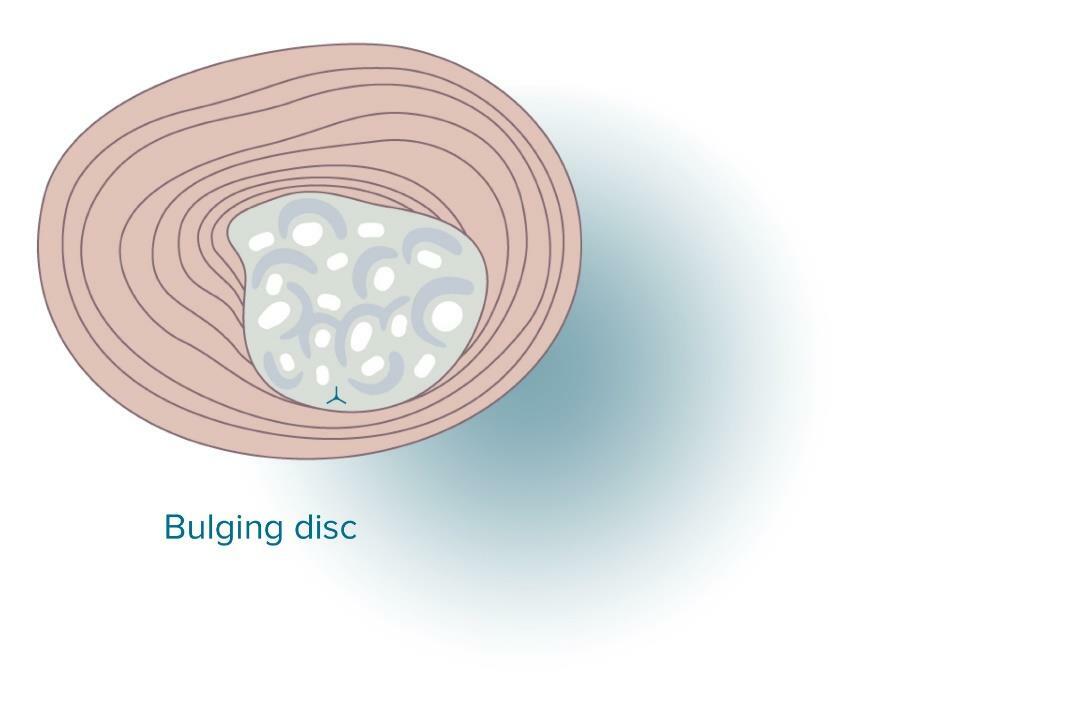
Bulging disc vs herniated disc
Unlike a herniated disc, when the nucleus pushes out of the annulus, a bulging disc protrudes outward with no impact on the outer layers of the annulus. In this case the disc goes into the spinal canal and can affect a nerve root. Disc bulge has one more name – disc prolapse. A bulging disc can be followed by a herniated disc. Signs of a bulging disc can be as follows: pain, weakness of the muscles, or numbness in the area of the bulge.
Sciatica vs herniated disc
Sciatica is a clinical term used to describe pain radiating down the leg. Sciatica is typically caused by a herniated disc. In this case, the spinal disc has herniated from its typical anatomical position and causes a compressed nerve root, which brings sciatica.
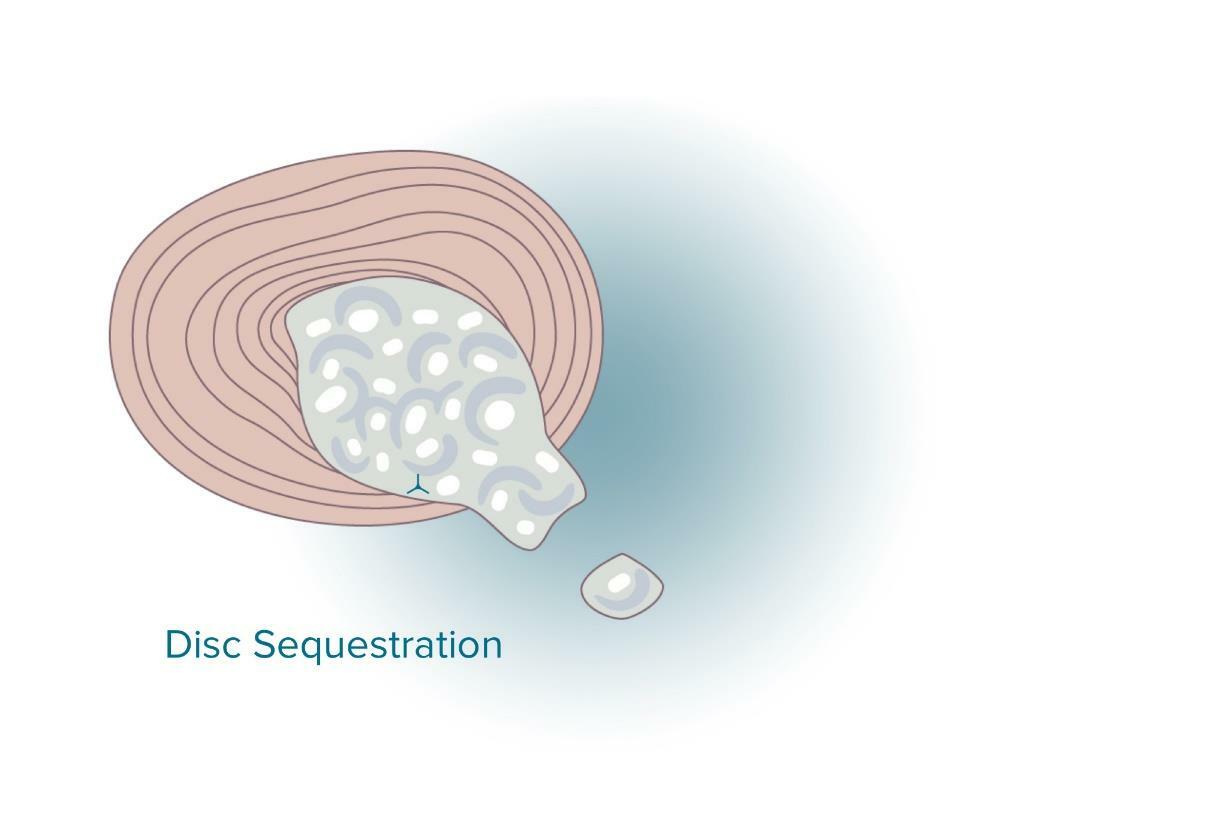
Sequestrated disc vs herniated disc
A sequestrated disc is a type of disc herniation. There are free fragments or pieces of a herniated disc. This free fragment, in other words a sequestered disc, can be found in the spinal canal and be the reason of the pressure applied to the spinal cord that can bring severe pain and injury.
Slipped disc vs herniated disc
A slipped disc is a term for an intervertebral spinal disc that is devoid of its standard shape and/or consistency. This can happen when nucleus pulposus or the soft inner material of a disc leaks out of its annulus fibrosus or external fibrous covering. A number of medical terms, including a herniated, ruptured, torn, bulged, or protruding disc, may be equally referred to a slipped disc.
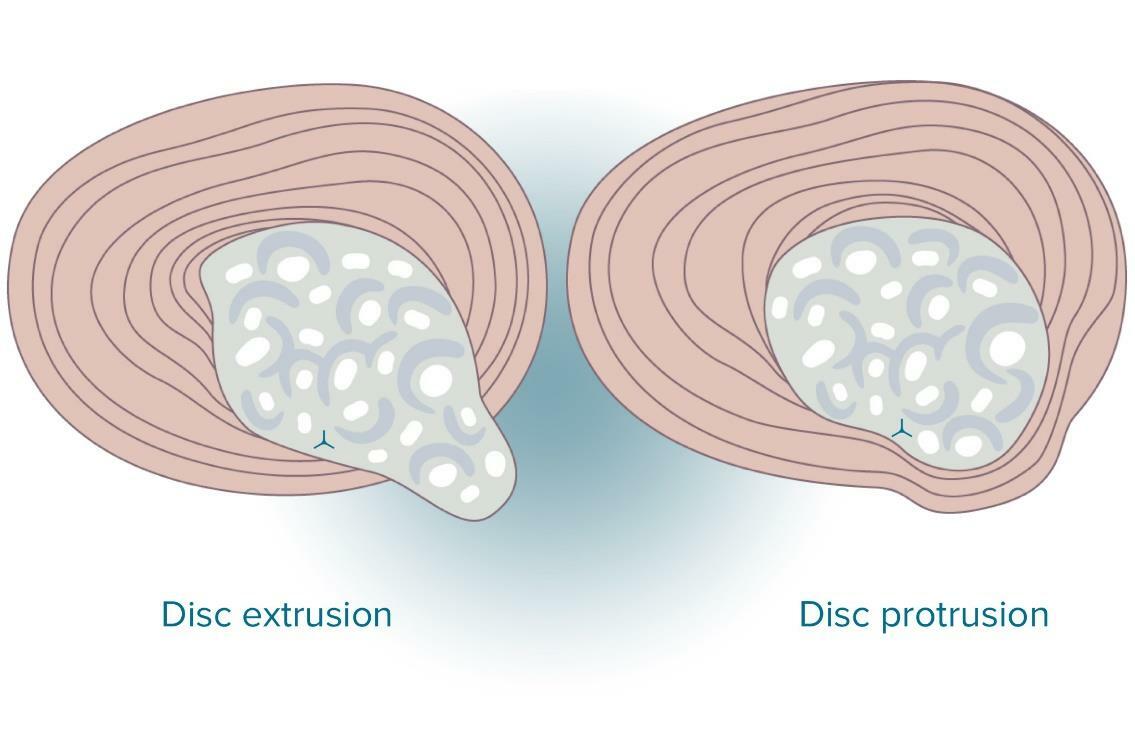
Disc protrusion vs herniated disc
Disc protrusions are a type of disc herniation when disc content goes beyond the normal confines of the intervertebral disc; a segment is less than 25% of the disc’s circumference. The base is wider than the largest diameter of the disc material which protrudes beyond the normal margins. The protrusion must stand within the limits of the particular vertebral endplates.
Disc extrusion vs herniation
An extruded disc differs from a disc protrusion - the base of the protruded material is narrower than its 'dome'. What is more, this material may go above or below the disc level.
Raptured disc vs herniated disc
A ruptured disc in back is one more definition for a herniated disc. However, this term is more popular to speak about an injury or trauma induced condition.
Disc degeneration
Aging triggers some chemical processed which weaken the intervertebral discs but do not cause their herniation. This has already been mentioned. Over time, the discs could dry out and may not be efficient in absorbing the shock from body’s movements. What is more, the discs can thin.
Disc thinning
The process of spinal disc thinning looks like a degenerative disc disease (it is an umbrella term for age-related disc wear), because discs progressively thin with age. To be more specific, the jelly-like nucleus (nucleus pulposus) contains less fluid over time, which can decrease the disc’s sponginess. Adding to this, the harder outer layer of disc (annulus fibrosus) may become brittle. Disc thinning can be accompanied with arthritis. This problem shortens discs, so that it damages spinal stability.
Pinched Nerve
A pinched nerve occurs when something within the body disrupts the work of a nerve by touching it. This nerve is usually located in one of the tight spaces within the body.
Tight space makes the nerves more vulnerable to being caught in these areas. The exit of the spine is one of these tightest areas.
This exit is composed of bones (vertebrae), discs, and ligaments. Typically, the exit is enough for the nerves to glide and slide within it.
However, if the exit is narrowed for any particular reason, this can result in a pinched nerve.
A herniated disc might be a common reason for a narrowed exit. If a herniated disc pinched nerve in different segments of the spinal vertebrae (ex. l4l5, l5s1), it can be manifested in different associated symptoms.
What Are the Symptoms of a Herniated Disc?
Any part of the spine is susceptible to herniation, although the lower back and neck (the lumbar and cervical spine) are the most common places for this disorder. Unlike the middle of the back (the thoracic spine), these are the flexible parts of the spine, provide many movements, thus they are highly likely to be exposed to wear and tear with the lost fluid volume.A patient might not experience any symptoms with minimal herniation or a lack of pressure on a nerve.
If herniations do affect nerves, patients could experience severe and unstoppable pain. The pain affects one side of the body and may radiate to an arm (with the herniated disc in the neck) or leg (with lumbar disc herniation; sciatica is an illustration of this).
A herniated disc has other manifestations:
- A dull ache on one side of the body
- Pain when coughing, sneezing, or moving into a certain position
- Numbness, tingling, or burning sensations due to a compressed nerve.
- Pain that worsens with sitting, but the symptoms can escalate when standing, walking, and bending
- Muscle weakness or spasm that may prevent a patient from lifting or holding different items
- Balance issues or limping due to weakness and/or pain
- Slow reflexes
- Difficulty getting up when seated
- Inability to stay still in one position for a long period of time
- Poor posture
- No bowel or bladder control (which can be an indicator for a cauda equina syndrome, a medical emergency)
Symptoms of slipped (herniated) disc in the neck
A cervical herniated disc can be painful or do not manifest any symptoms at all. The pain can be an ache in the neck, arm, and/or hand or electric-like pain radiating into these same areas. Sometimes, a person can experience arm or hand numbness or weakness. While some sort of trauma or neck injury may be the origin of a cervical herniated disc, the symptoms usually are spontaneous.
Cervical herniated disc pain and associated signs are likely to be felt in an arm. Symptoms are determined by the type of a herniated disc and a nerve root being pinched or inflamed. The pain, tingling, numbness, and/or weakness from the affected spinal cord can rarely be experienced in both arms or lower in the body. Loss of bowel and/or bladder control are not common but possible manifestations.
Symptoms of herniated disc in lower back
A lumbar herniated disc may have various symptoms—a moderate pain in the back and buttock or widespread numbness and weakness requiring immediate medical care.
A herniated disc typically presses against a neighboring nerve, which gives a radiating pain along the nerve. A lumber herniated disc is the most popular reason for sciatica, which is a leg pain along the sciatic nerve down the back of the leg.
Lumbar herniated disc pain is characterized as follows:
A pain in the leg. The leg pain is more severe than the low back pain. A patient can be diagnosed with sciatica or a radiculopathy if the pain radiates along the large sciatic nerve in the back of the leg.
Nerve pain. This is typically manifested as nerve pain in the leg. The patients say that the pain is burning, sharp, radiating, electric, or piercing.
Variable location of symptoms. The place of a herniated disc and the herniation degree give various symptoms in front or back of the thigh, the low back, buttock, foot and/or toes, the calf, and typically affect one side of the body.
Neurological symptoms. Patients typically experience numbness, weakness, a pins-and-needles feeling, and/or tingling in the leg, foot, and/or toes.
Foot drop. The condition described as foot drop is when a patient with a herniated disc may find it difficult to lift the foot when walking or standing on the ball of the foot.
Pain
Character- dull ache, burning, sharp, and piercing,
Pain radiates to hands, arms, feet, leg, and buttocks,
Pain is triggered by coughing, twisting, standing, sneezing, bending
Pain worsens at night.
What can cause a herniated disc
Disc herniation is most often caused by a progressive, aging-related wear and tear called disc degeneration. With age, discs are less flexible and more vulnerable to tearing or rupturing with even a slight strain or twist.Majority of people can't identify the cause of their herniated disc. One possible explanation is when a person exploits their back muscles instead of leg and thigh muscles when lifting heavy objects or twist and turn while lifting, this can cause a herniated disc. In rare occasions, do traumas, including a fall or a blow to the back, cause a herniated disc.
How to diagnose a herniated disc
If a patient would like to find out whether he/she has a herniated disc, the first thing to do is to consult a primary care doctor. A patient might be diagnosed with a herniated disc if a low back pain is accompanied by a radiating leg pain.The doctor is likely to ask the patient to do the “straight leg raise test.” Here, a patient lies down and lifts one leg straight up. If there is a herniated disc which affects a nerve, that movement will boost the compression and cause pain along the leg. The doctor also questions the patient about slow reflexes, numbness, and weakness.
The doctor asks the patient to undergo some imaging studies.
A common recommendation is to perform an imaging test before treatment. The purpose of this is to exclude any other possible reasons for fractures, tumors, infection, cauda equina syndrome, and other symptoms.
MRI is the most trustworthy tool to reveal a herniated disc.
- MRI (magnetic resonance imaging) accurately analyzes the lumbar spine area, spots a herniation site and the affected nerves.
- CT (computed tomography) scan can substitute an MRI when the latter is not possible for some reasons. However, this method does not predict the future effect of treatment.
- X-rays are helpful in diagnosing such problems as a broken bone, bone abnormalities, infection, tumor, or problems with the alignment of the spine. A herniated disc cannot be diagnosed with X rays only.
- Electromyography (EMG) can highlight the compressed nerve.
Treatment of slipped (herniated) disk
Most people with herniated discs are responsive to conservative treatment and do not need any surgery.What Are Nonsurgical Treatment Options for Herniated Discs?
To start with, a patient is recommended to adhere to a low, painless activity level for a few days to several weeks. This rule decreases the spinal nerve inflammation. Staying in bed is not the best recommendation for quick recovery.
Patients with a mild or moderate pain induced by a herniated disc are prescribed with nonsteroidal anti-inflammatory drugs. Patients with extreme pain might require an epidural steroid injection, which should follow instructions and X-ray manual to control the medication to the exact level of the disc herniation.
The doctor may advise physical therapy which is given further.
●Medication
A painful herniated disc is typically treated with over-the-counter (OTC) medications, such as non-steroidal anti-inflammatory drugs (NSAIDs). Opioids, tramadol, and/or corticosteroids could be prescribed for more severe pain.
Pain medications are taken orally in tablets, capsules, and liquids. The examples of pain killers are given below:
●Local pain relievers
Key pain relief medications are creams, gels, or patches which are applied to the skin. They can be prescribed by a doctor and/or bought over-the-counter with no prescription. Their task is to relieve the localized pain.
Counterirritants include such ingredients as menthol, wintergreen, and eucalyptus, which give a hot or cold feeling. Counterirritant creams and gels often treat sore muscles and are safe enough to be taken with other forms of pain killers. Some counterirritants, for example products with menthol, are sold as skin patches.
Lidocaine is a local anesthetic cream, gel, or skin patch that can temporary numb, minimize pain in the area it is applied on. Lidocaine is often taken together with other ingredients in the over-the-counter products. Versatis 5% medicated Plaster is one of the most popular one among the patients.
NSAID-containing ointments and gels (diclofenac, voltaren gels, finalgel, etc.) are helpful for acute back pain, including pain, swelling, inflammation.
●Acupuncture
Acupuncture could be considered as an efficient tool to relieve pain, to improve quality of life and productivity. The nerves in muscles and other tissues are stimulated by inserting fine needles. This action triggers the release of endorphins and other neuro-humoral factors. Acupuncture is proven to decrease inflammation by contributing into the release of vascular and immunomodulatory factors and by increasing local microcirculation. This may also enhance better joint movements and relief of muscle stiffness.
●Physical therapy
Special exercises and physical therapies can be practiced to treat the pain from a slipped disc.
●Therapeutic physiotherapy with the focus on physiotherapy. Laser therapy, magnetotherapy, phono- and electrophoresis are the most effective and health-supporting means for a herniated disc.
●Chiropractic manipulation
A raptured disc pain may be treated by chiropractic manipulations applied to the lumbar spine. A chiropractor is seen to be a health care profession which treats disorders in the nervous system and/or musculoskeletal system in a non-surgical manner. Chiropractors practice spinal manipulations and treat neighboring structures. When chiropractors deal with the patients with non-specific chronic low back pain, the long-term effects are pronounced by spinal manipulations after the initial intensive manipulative therapy. However, if a patient is diagnosed with a disc herniation, he/she should avoid manipulation of the affected segment. This might enlarge hernia or change its localization, thus exacerbating the pathological process.
●Self-care
If a patient strives to promote healing and/or prevent a problem disc segment from worsening, he/she should stay away from:
• Constant spine bending
• Unexpected, abrupt movements, for example jumping
• High-intensity exercise and lifting heavy items
Avoid pressure on the spine.
What is more, a pro- active lifestyle, moderate physical exercising, no smoking and weight loss in obese people can reduce the risk of herniation and associated problems.
- Diet: review a diet especially if a patient had extra weight. In any case, healthy food is a must for everyone.
- Hydration: drink much water. If a herniated disc compresses a nerve, any dehydration in that disc will exacerbate the condition.
- Overall activity: be active. Walk as much as possible, but don’t overdo this activity. Stop if you experience some pain, have a break, and then continue walking.
- Sleep: sleep is one of the key components of a recovery from a herniated disc–healing occurs with proper sleep. No ample sleep each night can give no result.
What Surgical Procedures Treat Herniated Discs?
If a patient has tried non-surgical therapies and still has no result after several months, surgery may be an alternative treatment. This is usually a one-hour outpatient procedure.
There are two main surgical procedures to treat a lumbar herniated disc.
Microdiscectomy. Portions of the disc are removed to relieve the pressure on the spinal column. Microdiscectomy is also coined as microdecompression.
Laminectomy. In a laminectomy, a portion of the vertebral bone is removed. This gives more space for the spinal cord and nerves, so they aren't compressed any longer.
We have two extra options for herniated discs in the cervical spine (the neck)
Anterior cervical discectomy and fusion (ACDF) or cervical disc replacement (CDR)
ACDF or CDR are surgeries designed to remove the affected disc and insert either a bone graft (ACDF) or artificial disc (CDR) to maintain stability in the area.
Microlaminoforaminotomy
In this case, a surgeon removes a small piece of bone from a vertebra, which creates more space for the pinched nerve(s).
Surgeries typically make most patients feel relief from symptoms like pain, numbness, and weakness right away. However, full recovery could take several weeks or months.
Alternative treatments for a slipped disc
We are born with such a physiological process as resorption. Spontaneous resorption of the herniated disc was firstly mentioned in the academic studies 37 years ago. Resorption therapy is a new alternative method which is still not popular and extensively attacked by many professionals. Resorption is underestimated. This process accelerates with a range of procedures, which increases blood supply, metabolism, and alleviates acute pain.
This treatment method was firstly popularized by Tkachev & Epifanov Clinic, a Russian Clinic.
Read more
How to prevent a slipped disc
Preventive measures for a herniated disc are as follows:Exercises. Stronger trunk muscles stabilize and maintain the spinal cord.
Good posture. This applies less pressure on spine and discs. Keep your back straight and aligned, particularly in a sitting position for long periods. Lift heavy items properly with your legs — not your back — being involved into this work.
Healthy weight. Excess weight puts more pressure on the spine and discs. Obesity makes the discs vulnerable to herniation.
No smoking. Don’t use any tobacco products.
FAQs
Can a bulging disc become a herniated disc?Yes. A bulging disc is considered to accompany natural aging, but it has different severity degrees. A herniated disc occurs when a crack in the hard cartilage releases the inner soft tissue from its limits.
Does numbness from herniated disc go away
This problem is solved with the right treatment.
Can a herniated disc heal naturally
Yes, absolutely, but not in all cases. Read more
How to relieve herniated disc pain in lower back
Herniated discs are a common problem. In many cases, conservative, non-invasive treatment methods are likely to be prescribed first. They work to relieve painful symptoms while the body recovers. You can’t replace your shock absorption system, but stretches and exercises developed for herniated discs can accompany other conservative treatment methods to get rid of pain and discomfort of a herniated disc.
Read above Treatment of slipped (herniated) disk
Slipped disc recovery time
Many factors determine the recovery time for a herniated disc. It depends on you lifestyle, your job, severity of your hernia, its size, treatment, and many other factors.
